Cataract is a common eye issue that can be treated. Cataracts are caused by a build-up of proteins in your eye. Consequently, your lens gets cloudy and blurry. This is a natural age related occurrence that, unfortunately, happens to many people as they age. In fact, more than half of those over 80 years old will experience some form of cataract.
Cataract surgery is a very common procedure that has been made safe and effective over the years. In fact, it is one of the most commonly performed surgeries in the world. Cataract surgery is a procedure that can be done on an outpatient basis by a cataract specialist. It usually only takes around 10 to 15 minutes from beginning to end.
1
Indications for Cataract Surgery
 While cataracts are commonly found in older individuals, they do not always indicate anything is wrong. In fact, many people who have cataracts do not experience any sort of symptom. If you are told you have a cataract, but it is not causing any trouble in your daily life, your doctor may tell you there is no need to do anything about it and that they will keep an eye on it. That said, if you are starting to have difficulty reading or experiencing other problems that are impacting your day-to-day activities, it may be time to consider surgery to remove the cataract.
While cataracts are commonly found in older individuals, they do not always indicate anything is wrong. In fact, many people who have cataracts do not experience any sort of symptom. If you are told you have a cataract, but it is not causing any trouble in your daily life, your doctor may tell you there is no need to do anything about it and that they will keep an eye on it. That said, if you are starting to have difficulty reading or experiencing other problems that are impacting your day-to-day activities, it may be time to consider surgery to remove the cataract.
2
Cataract Removal
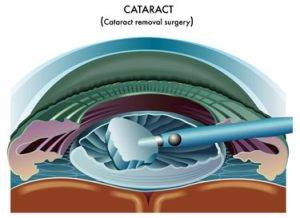
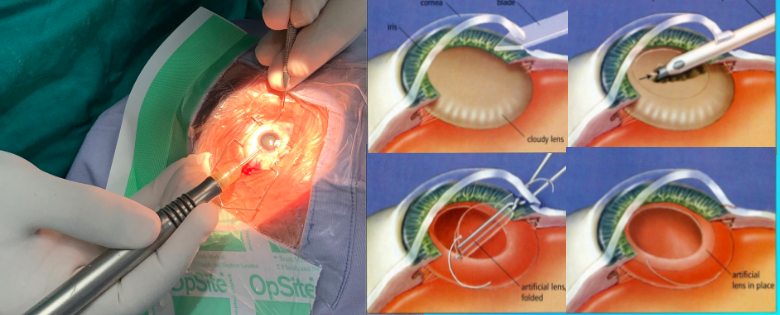
Cataract surgery involves removing the cloudy lens and replacing it with an artificial lens. It is a major surgery so it’s important to make sure you have a trained surgeon that you can trust to do the job right.
A common surgical method is Phacoemulsification and the other standard one is Extracapsular Cataract Extraction (ECCE). Phaco involves surgically removing the cloudy lens and replacing it with an artificial lens. ECCE is a surgery that may be necessary if the cataract is hard.
3
Why Choose Us
 It is important to do your research when looking for a doctor to perform cataract surgery. Scrutinize the physician's credentials and patient testimonials to determine if they are right for you. In addition, choose a clinic with knowledgeable and caring staff members in order to find the best doctor for cataract surgery.
It is important to do your research when looking for a doctor to perform cataract surgery. Scrutinize the physician's credentials and patient testimonials to determine if they are right for you. In addition, choose a clinic with knowledgeable and caring staff members in order to find the best doctor for cataract surgery.
Acuity Eye Center is known for providing high-quality care for patients needing cataract surgery in Pakistan. The clinic makes every patient feel like part of the Acuity family from the moment they walk through the doors.
Dr. Zia ul Mazhry at Acuity Eye Center is a specialist in Cataract Surgery with more than 3 decades of experience in the field of Ophthalmology. He has got his post-graduation from Royal College of Surgeons Edinburgh Glasgow and College of Physicians and Surgeons of Pakistan. He uses cutting edge technology and a variety of intraocular lenses to provide high quality treatment at an affordable price to everyone in need. Evidence based approach is used right from evaluation and planning to exercising the plan and the post procedure care. Generally speaking, Dr. Zia ul Mazhry and his staff are dedicated to providing affordable, high-quality cataract care to their patients.
Frequently Asked Questions (FAQs)
Is cataract surgery the only treatment for cataracts?
When a person has cataract, the lens in their eye is damaged and can no longer be repaired. The only way to fix the person's vision is to replace the natural lens with an artificial intraocular lens. This means that surgery is required.
Can eye drops prevent or cure cataracts?
No, you cannot reverse cataracts without surgery. Currently, there is no non-surgical cure for cataracts.
Can cataracts be prevented or reversed?
If you get a pair of eyeglasses, they may help improve your vision while the cataract is still in its early stages. Just keep in mind that as your cataract gets larger, it will start to cloud more and more of your eye's natural lens. And when it gets to the point where your vision is starting to interfere with your daily activities, that's when you'll want to consider surgery as the best option for restoring most of your vision and improving your quality of life.
Can a cataract come back after surgery?
Cataract surgery completely removes your natural lens. So, it is actually impossible for cataracts to grow back after surgery. However, you should be aware of a condition known as “secondary cataract” or “after-cataract” that can occur following cataract removal.
What is a "secondary cataract"?
A secondary cataract, otherwise known as Posterior Capsule Opacification (PCO), is a relatively common complication post-cataract surgery. It's caused by the overgrowth of epithelial cells and results in reduced vision. The only way to get rid of secondary cataracts is via YAG laser capsulotomy - a quick, easy outpatient procedure that takes no more than a few minutes.

